West Texas #1 Dry Eye Treatment Center
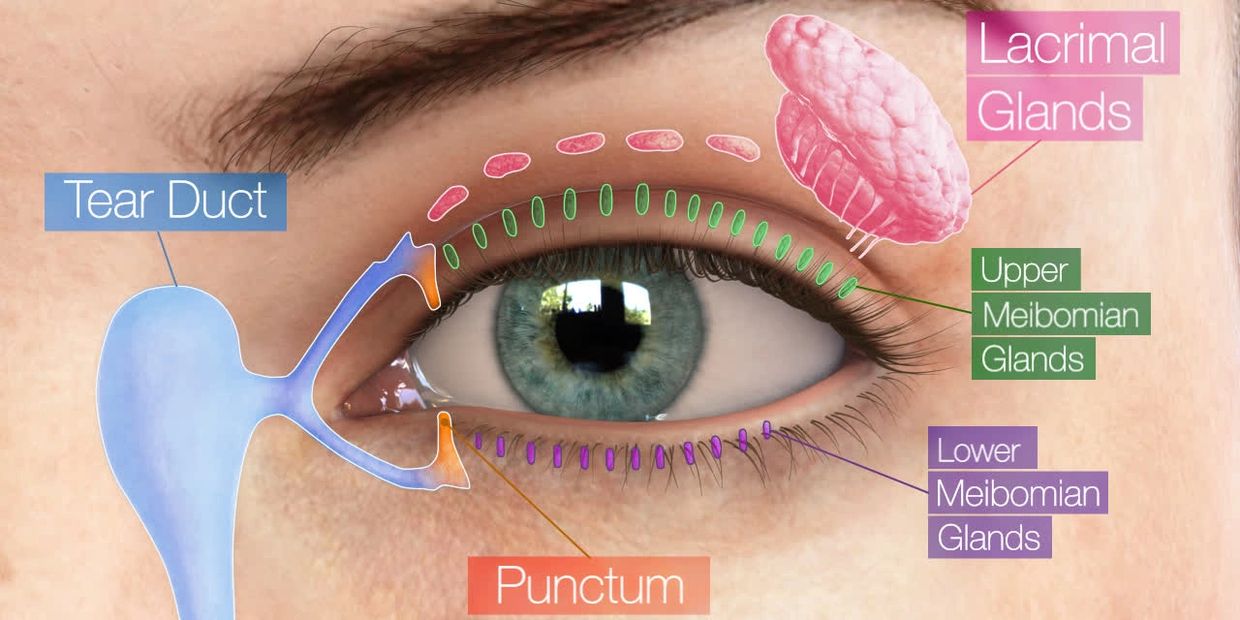
TEAR PRODUCTION MODEL
TREATMENT OPIONS
ARTIFICAL TEARS

Artificial Tears
For mild cases of dry eyes caused by computer use, reading, schoolwork and other situational causes, the best dry eye treatment may simply be frequent use of artificial tears or other lubricating eye drops. Artificial tears usually are the first step in dry eye treatment. There are many brands of artificial tears that are available without a prescription. The challenge with using artificial tears is not lack of product availability - it's the confusing number of brands and formulations available to choose from. Artificial tears and other over-the-counter (OTC) lubricating eye drops are available in a wide variety of ingredients and viscosity ("thickness").
If your eye doctor recommends that you use one or more brands or formulations of artificial tears, be sure to follow the directions he or she gives you concerning when and how often you use them. Also, do not substitute other brands from those your eye doctor recommends. Using a different brand or multiple brands of artificial tears will make it difficult to assess the success of the dry eye treatment your doctor recommended.
STEROIDS

Steroid Eye Drops
Over the past several years, inflammation has been recognized as a significant cause of dry eyes. Inflammation frequently causes the redness and burning associated with dry eye disease. Artificial tears usually do not adequately address these inflammatory changes, and your doctor may recommend steroid eye drops to better manage the underlying inflammation associated with dry eyes. Steroid eye drops generally are used short-term to quickly manage symptoms. They often are used in conjunction with artificial tears and Restasis or Xiidra, as a complement to these more long-term dry eye treatment strategies. Steroid eye drops (especially if used for relatively long periods) have the potential of causing side effects. So, it's important to make your eye doctor aware of your full medical history before starting steroid eye drops. For example, steroid eye drops can increase the risk of developing high eye pressure or even cataracts if used for extended periods of time. But these risks are low when the drops are used only on a short-term basis for dry eye treatment.
PRESCRIPTION EYE DROPS

Restasis
Instead of OTC artificial tears (or in addition to them), your eye doctor might recommend daily use of a prescription eye drop called Restasis (Allergan) for your dry eye treatment. Restasis does more than simply lubricate the surface of your eye. It includes an agent that reduces inflammation associated with dry eye syndrome and helps your body produce more natural tears to keep your eyes moist, comfortable and healthy. It's important to know, however, that the therapeutic effect of Restasis is not immediate. You must use the drops daily for a minimum of 90 days to experience the full benefits of this dry eye treatment. Some people who try Restasis will experience burning eyes early during the first few weeks of treatment.
Xiidra
Xiidra (ZYE-druh) is another prescription eye drop for dry eye treatment. Xiidra (Shire), like Restasis, is aimed at reducing inflammation associated with the signs and symptoms of dry eyes. The safety and efficacy of Xiidra was studied in four placebo-controlled, 12-week clinical trials that included 1,181 people with dry eyes. Participants were evaluated for dry eye signs and symptoms just prior to starting use of the drops, then after two weeks, six weeks and 12 weeks of Xiidra use. In two of the four studies, participants noticed a significant reduction in dry eye symptoms after using Xiidra for two weeks. In all four studies, participants noticed a larger reduction in dryness symptoms after six weeks and 12 weeks of Xiidra use. Also, at 12 weeks, a statistically significant reduction in signs of dry eyes was found among Xiidra users compared with participants given a placebo in two of the four studies. The most common side effects of Xiidra reported in the studies were eye irritation, altered taste sensation and reduced visual acuity, which occurred in 5% to 25% of participants. The recommended dosage for Xiidra, like Restasis, is two applications in each eye per day, approximately 12 hours apart.
PRESCRIPTON NASAL SPRAY

Neurostimulation
Tyrvaya is a highly selective cholinergic agonist that binds to cholinergic receptors with high affinity.
It activates the trigeminal parasympathetic pathway, accessible within the nose, resulting in enhanced basal or natural tear film production.
ORAL MEDICATIONS

Doxycycline
Due to its anti-inflammatory characteristics and its ability to improve oil gland function, it is the most effective medication available for the treatment of meibomian gland dysfunction. Meibomian glands produce the oil layer of the tear film and help prevent tears from evaporating too quickly.
Doxycycline 100 mg once daily or twice daily may be given for meibomian gland dysfunction (MGD), if indicated, followed by a supervised decrease in dosage to as low as 20 mg PO QD. Topical cyclosporine 0.05% ophthalmic emulsion is effective FDA-approved treatment for dry eye disease.
Of course, doxycycline has several side effects, and should be taken with some caution. Many of the side effects are related to the gastrointestinal health, such as loss of appetite, nausea and vomiting, diarrhea. People may also get sensitivity to the sun, so sun protection while using this medication is recommended.
OMEGA - 3

Omega-3 fatty acids include alpha-linolenic acid (ALA), DHA, and EPA. Since ALA does not efficiently convert to EPA and DHA in the body, EPA and DHA are most commonly found in fish and fish oils where research shows that supplementing with these omega-3s dramatically reduce prostaglandin formation, downregulate proinflammatory gene expression, and inhibit and reduce neutrophil entry to sites of inflammation.
INTENSE PULSE LIGHT THERAPY

IPL
Intense pulsed light (IPL) has long been used to treat rosacea on the skin. Rosacea on the skin and eyelid often occur together.
Ocular rosacea is characterized by dilated blood vessels coursing along the eyelash margin in patients suffering from blepharitis and may contribute to dry eye symptoms.
In IPL treatment, a hand-held device flashes bright light onto the skin. The light is filtered to allow only wavelengths that can be absorbed by the dilated blood vessels. The effect of this treatment may be the resolution of the dilated vessels and associated inflammation that contributes to dry eye symptoms.
Many patients experience relief from their dry eye symptoms after IPL and become less dependent on artificial tears and other routine measures to keep their eyes comfortable. For this reason, IPL treatment may be well-suited for dry eye patients who don't want to be troubled by the inconvenience of frequent eye drop use.
IPL treatment generally is not covered by health insurance or vision insurance and it may not be appropriate for patients with certain skin pigmentations.
ENVIRONMENTAL CHANGES

Maybe it's just a small shift in your surroundings -- a change of seasons or a new office. But suddenly, your eyes constantly feel dry.
It’s not your imagination. Your environment can trigger dry eye disease or make it worse. Luckily, if you can figure out what’s irritating your eyes, you may be able to make changes to ease the discomfort. If you have long-lasting symptoms of dry eye, your doctor can also prescribe treatments.
How Can Your Environment Cause Dry Eye?
Dry eye disease happens when your tears don’t lubricate your eyes well enough. This can happen if your eyes don’t make enough tears. But it can also happen if your tears evaporate too quickly from the surface of your eyes. That's the process that changes in your environment can affect.
Warm or dry air makes moisture evaporate from the surface of your eyes more quickly than cool or humid air. This means people in hot, dry climates are more prone to dry eye disease year-round than those in wet, tropical areas.
But colder weather can also trigger dry eye. That's because outdoor humidity often drops in the winter. And using the heating system in your home or office during the winter can make your indoor environment very warm and dry.
Pollution and Dry Eye
Your eyes are exposed to whatever is in the air around you, whether that’s clean mountain air, city pollution, or smoke from a fire.
Tiny, solid particles in air pollution, dust, and smoke can lodge themselves in your tear film, the moist layer of tears that coats your eye. This means the tear film is less able to keep your eye lubricated, which makes your eyes feel dry.
Also, pollutants that end up on the surface of your eyes can trigger inflammation, your immune system’s natural reaction to dust, dirt, and germs. In turn, inflammation affects the way the cells in your eyes work. That can lead to less tear production, too.
Indoor Environment and Dry Eye
Many of the things that influence dry eye disease indoors are the same as those that affect it outside: temperature and humidity. Spending time in a warm, dry room is more likely to cause dry eye than a cool, humid room. Poor air quality, whether from indoor pollution, dust, cigarette smoke, or aerosol sprays, is also linked to dry eye.
Of course, it's easier to change your indoor environment than the one outdoors. Adding a humidifier to your home or office, or lowering the temperature by just 1 degree, can decrease symptoms of dry eye. You can often improve air quality by opening windows, cleaning surfaces and air vents regularly, and growing plants indoors.
Travel and Dry Eye
Airplanes are notorious for dry air and poor air quality. Passengers and crews often report not only dry eyes, but dry skin and dry or stuffy noses after flights. Studies mimicking the conditions on airplanes have shown that the level of humidity on a flight makes tears evaporate from your eyes faster.
AMNIOTIC MEMBRANE

Amniotic Membrane (AM)
Amniotic membranes are placed directly on the front of the eye, and provide not only a nourishing and protective barrier to help facilitate corneal health, but can also provide rejuvenating stem cell contributions to the cornea and prevent future corneal damage due to dryness.
Amniotic membranes are part of the newest treatment methods used to approach symptoms of moderate to severe dry eye disease, as well as many other ocular surface conditions. These complex medical devices are derived from ethically sourced amniotic tissue that not only provides the front of the eye with a protective and nourishing barrier, but also delivers regenerative and healing properties to damaged corneal tissue. While they have gained a lot of popularity in their role for treating severe ocular surface diseases, such as recurrent corneal erosions or chronic ocular surface infections, they can also play a significant role in the treatment and management of dry eye disease.
The Basics of Amniotic Membranes
Amniotic membranes are ocular grafts that are derived from the innermost layer of the placenta. This tissue is rich in stem cells, which can provide a damaged ocular surface with important regenerative properties. They are ethically sourced, and only donors that meet very strict health standards are able to donate tissue that can be repurposed for an amniotic membrane. When this membrane tissue is used on the eye, it is formulated into a large diameter graft that is secured by a round flexible plastic ring. During treatment with an amniotic membrane, this plastic ring is inserted between the eyelids, so the nutrient-rich tissue rests directly on the front surface of the eye. Within a few days, the graft beings to dissolve and the regenerative properties of the stem-cell-abundant tissue is absorbed within the ocular surface so tissue healing can begin to occur. After a few days, the membrane and plastic ring are removed. However, the healing properties do not stop there. Amniotic membranes typically allow for regeneration of damaged tissue long after the actual graft is removed. The process of applying and removing an amniotic membrane is quick and pain free. It is an in-office procedure done by an eye care professional within minutes. Your doctor will insert a numbing drop to prevent any discomfort, then gently insert the flexible plastic ring under the eyelids of the eye receiving treatment. The eyelids are then typically taped shut for a short period of time to keep the graft in place. The membrane is not painful during the treatment time, and within a matter of days (usually 3-10 days, depending on severity of disease), the graft and the plastic ring are quickly and easily removed by your doctor. The simple procedure carries very little risks, but allows for many healing benefits.
Uses for Amniotic Membranes
Amniotic membranes can be used in the treatment and management of many ocular surface diseases. For patients who experience painful recurrent corneal erosions, amniotic membranes may be a method of not only reducing symptoms of a current episode, but also providing the eye with healing properties to avoid another incident. They can be used in cases of long-term ocular inflammation in which the front surface of the eye is negatively affected. They may also be useful in treating moderate to severe dry eye disease, in which traditional treatment methods have proven to be ineffective. These powerful tissues have proved to be widely useful in promoting a healthy ocular surface.
ADJUST MEDICATIONS

Medication adjustment.
Many medicines — including antihistamines, antidepressants, birth control pills, certain blood pressure medications and more — can cause or worsen dry eye symptoms.
Even over-the-counter (nonprescription) medications for allergies and other conditions can cause dry eyes.
Be sure to discuss all medications you are taking with your doctor if you are experiencing dry eye problems.
However, never discontinue a prescription medication without first discussing it with your physician.
LACRISERT

Lacrisert
Lacrisert (Bausch + Lomb) is a sterile, slow-release lubricant that is placed under the lower eyelid where the conjunctiva of the inside of the eyelid meets the conjunctiva of the eyeball. It is a solid insert composed of a preservative-free lubricating agent (hydroxypropyl cellulose) that slowly liquefies over time, providing an all-day moistening effect. For most people with dry eyes, a single Lacrisert is applied once a day. The device has been proven to relieve dryness, burning, watery eyes, foreign body sensation, itching, light sensitivity and blurred vision, according to the company. Lacrisert typically is recommended for patients with moderate to severe dry eye symptoms, especially if dry eye treatment with artificial tears alone proves unsuccessful. If placed under the eyelid improperly, it's possible Lacrisert can cause a corneal abrasion. Also, Lacrisert may cause transient blurred vision, eye discomfort or irritation, matting or stickiness of eyelashes, red eyes and sensitivity to light.
PUNCTAL PLUGS

Punctal plugs
Punctal plugs sometimes are used in dry eye treatment to help tears remain on the surface of the eye longer.
A punctal plug is a small, sterile device that is inserted into one of the small openings (puncta) of tear drainage ducts that are located in the inner corner of the upper and lower eyelids.
After these openings have been plugged, tears can no longer drain away from the eye through the ducts. This results in the tear film remaining intact longer on the surface of the eye, relieving dry eye symptoms.
So where do the tears go? Usually they will simply evaporate from the eye surface without symptoms. But if insertion of punctal plugs causes watery eyes, one or more of the plugs can be removed.
SELF HELP

Blink more often
Research has shown that people tend to blink much less frequently than normal when viewing a computer, smartphone or other digital display. This decreased blink rate can cause or worsen dry eye symptoms. Make a conscious effort to blink more often when using these devices. Also, perform full blinks, gently squeezing your eyelids together, to fully spread a fresh layer of tears over your eyes.
20-20-20 Eye Rule
Take frequent breaks during computer use. A good rule of thumb here is to look away from your screen at least every 20 minutes and look at something that is at least 20 feet from your eyes for at least 20 seconds. Eye doctors call this the "20-20-20 rule," and abiding by it can help relieve dry eyes and computer eye strain.
Thoroughly remove eye makeup.
Eyeliner and other eye makeup can clog the openings of the glands at the base of the eyelashes, leading to meibomian gland dysfunction and evaporative dry eye. At the end of the day, be diligent about removing all makeup from your eyelids and eyelashes.
Clean your eyelids
When washing your face before bedtime, gently wash your eyelids to remove bacteria that can cause blepharitis and meibomian gland problems that lead to dry eye symptoms. Apply a warm, moist washcloth to your closed lids for at least 20 seconds. Then gently wash your lids and lashes with a mild cleanser, such as diluted baby shampoo or pre-moistened eyelid wipes sold in drugstores.
Wear quality sunglasses
When outdoors in daylight hours, always wear sunglasses that block 100% of the sun's UV rays. For the best protection, choose sunglasses that also feature a wrap-style frame to protect your eyes from wind, dust and other irritants that can cause or worsen dry eye symptoms.
Use a humidifier
Dry air inside your home, particularly in dry climates, or in cold climates in winter, can contribute to making your eyes dry. Consider adding a humidifier to increase the relative humidity inside your home.
STOP WEARING CONTACTS

Discontinuing or reducing contact lens wear
If you wear contact lenses, it can be difficult to tell if an underlying dry eye condition is causing contact lens discomfort or if your contact lenses are causing dry eye symptoms. If you wear contacts, it's often best to discontinue wearing them (or perhaps switch to daily disposable contact lenses) while your dry eye treatment is in progress.
AUTOLOGOUS SERUM
AUTOLOGOUS SERUM

Autologous Serum Eye Drops
Autologous serum eye drops are unpreserved, are nonantigenic by nature, and contain growth factors, fibronectin, immunoglobulins, and vitamins at concentrations similar to or higher than those in natural or artificial tears. Serum eye drops are used for severe dry eye disease with punctate epithelial defects and corneal damage to promote reepithelialization. They can be used successfully in patients who are refractory to other forms of treatment.
This website uses cookies.
We use cookies to analyze website traffic and optimize your website experience. By accepting our use of cookies, your data will be aggregated with all other user data.